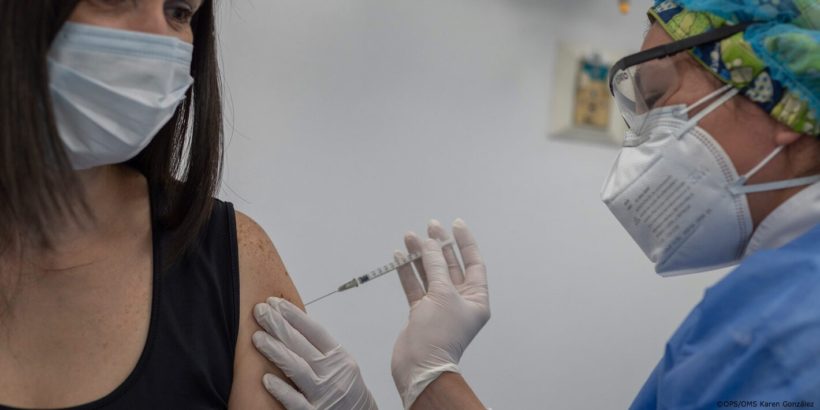The World Health Organisation (WHO) estimates that at least 70% of the population must be vaccinated in order to legitimise the end of the Covid-19 pandemic. This would equate to 5.4 billion people immunised, and if we take into account that a second dose is required, the demand will considerably exceed the initial supply.
The race for a vaccine has been a business opportunity for biotech and pharmaceutical companies. During 2020, 2021 and 2022 they will have added US$60 billion to their turnover, according to Bloomberg.
The scope of biotech companies is greater because they obtain patents for 12 years, while pharmaceutical companies generally have the rights for five years. This generates very subtle profits for biotech’s that have to operate at a loss for some time, until some highly profitable factor such as the Covid-19 vaccine comes along. This explains why there are strategic alliances between them.
The biotech companies that initiated the vaccine work were BioNTech, CureVac, Novavax, Janssen, Serum Institute of India and Moderna among others. The pharmaceutical companies are: Pfizer, AstraZeneca, Johnson & Johnson, Sanofi and GlaxoSmithKline (GSK).
They were joined by Bayer through a business deal with CureVac. The German brand powerhouse, which owns Aspirin, has global distribution logistics that no laboratory in the world possesses.
The clearest case of growth will be for Germany’s BioNTech, partnered with US drugmaker Pfizer, which in phase III demonstrated 95% efficacy. This alliance is expected to have a turnover of six billion dollars by 2021.
On the other hand, Moderna, a US company, will make a big leap in revenue. Its vaccine, whose manufacture was awarded to the Madrid-based laboratory Rovi, is the most advanced in terms of timelines. Preliminary results indicate an efficacy of 94.5%.
Revenues are estimated to reach US$5 billion. Novavax (which also has a vaccine in phase III), will reach US$1 billion and CureVac will be the big surprise in 2022, with US$1.2 billion according to forecasts.
It is key to remember that these companies have received millions of dollars in direct grants for vaccine R&D or in supply contracts from the EU and the US.
The US, EU and UK oppose the proposed exemption of intellectual property rights and patents for the Covid-19 vaccine. The proposal was submitted to the World Trade Organisation (WTO) in October 2020 by South Africa and India, and has already been joined by more than 100 countries. It consists of eliminating intellectual property barriers so that companies can transfer their technology and know-how to other production plants to mass-produce all the doses required to immunise the world’s population as quickly as possible. According to Tedros Adhanom, director of the WHO, this production capacity is available.
The Agreement on Trade and Intellectual Property Rights (TRIPS) signed by the member countries of the WTO is nothing more than the legal creation of monopolies insofar as it grants capital the exclusive right, for years, to produce and market a good. They argue that patents are the only guarantee to encourage investment in research and development.
With the blackmail of the incentive, what they really give to the pharmaceutical companies is the power to decide who lives and who dies, as well as deciding what we will live and what we will die from. They set the research agenda according to what is most profitable for them.
Following Curcio (2020), research funding does not even come from the private pharmaceutical industry itself. It is governments that have historically provided the financial resources and it is in universities and mainly public institutions that research has been developed and then appropriated by pharmaceutical companies. Of the US$13.9 billion that has gone into Covid-19 vaccine research, governments have provided US$8.6 billion, non-profit organisations US$1.9 billion, while only US$3.4 billion has been provided by private pharmaceutical companies, just 25 percent. To this we must add the secure market for the vaccine, in fact, by December 2020 the governments of the so-called developed countries had pre-ordered 10.38 billion doses.
The US pharmaceutical company Moderna developed the Covid-19 vaccine with entirely public funding, receiving US$562 million. It was pre-ordered 780 million doses at an average price of around US$31 per dose, generating revenues of US$24 billion. You do the maths on the company’s profit.
Pfizer/BioNtech, received US$268 million from the government, about 66 per cent of what it spent on research. It was pre-ordered 1.28 billion doses, which at an average price of $18.5 per dose equates to revenues of $23.68 billion. British-owned AstraZeneca/Oxford, pre-ordered 3.29 billion doses, which it sells at a price of US$6 per dose, will earn US$19.74 billion in revenues, but 67 per cent of the US$2.2 billion it spent on research was public. Johnson&Johnson was ordered 1.27 billion vaccines, which it sells at US$10 per dose for US$12.7 billion in revenue, having made an investment of US$819 million with 100 per cent public funding.
Vaccine prices range from US$4 to US$37 per dose: Sputnik-V, US$10; Sanofi/GSK between US$10 and US$21; Novavax 16; Moderna between 25 and 37; Sinovac between US$13 and US$29, in addition to those already mentioned.
The vaccine against Covid-19 is a round business, apparently the best of these times: the investment for the research was assumed by the governments that gave the resources to the private pharmaceutical companies; they have the market guaranteed because the same governments pre-ordered the vaccines to the companies they financed; all the profit goes to the pharmaceutical companies, mostly private, which are also the ones that, thanks to the monopoly granted by the same governments through the TRIPS, have the exclusivity of production and commercialisation for years.
This restriction of access to the vaccine, a consequence of patents, occurs while 500,000 people are infected and 8,000 die every day from the disease. Is this, or is this not, the most inhumane example of capitalism?
According to Oxfam (2021), while the highest income countries vaccinate one person per second, most countries have yet to provide a single dose. Of the 128 million doses of vaccines administered to date, more than three quarters have been administered in just 10 countries that account for 60 per cent of global GDP. Nearly 130 countries, with 2.5 billion people, have not yet started vaccination. It is estimated that by mid-2021, only 3 per cent of the population of the poorest countries will have been vaccinated, and at best one-fifth by the end of that year, which in turn will delay not only the economic recovery of these countries but also the living conditions of their populations. The US has received 25 per cent of all vaccines available globally and the EU 12.6 per cent.
The US, the EU and the UK are so brazen that they refuse to exempt patents in order to favour their pharmaceutical capital, despite the fact that in 2001 they agreed within the WTO to relax intellectual property rights in case of public health emergencies: “We agree that the TRIPS Agreement does not and should not prevent members from taking measures to protect public health. Accordingly, while reiterating our commitment to the TRIPS Agreement, we affirm that the TRIPS Agreement can and should be interpreted and implemented in a manner supportive of WTO Members’ right to protect public health and, in particular, to promote access to medicines for all”.
The governments of the world’s central states have embarked on this deadly game. Having largely financed the development of vaccines, they were also the first to be able to administer them to their populations, to the extent that they wanted to be vaccinated. The first and for the moment the only ones. Indeed, despite their regularly renewed commitments to the contrary, their contribution to making vaccines available to the populations of the world’s periphery through the Covax system, set up by the WHO in partnership with the NGO Gavi, has so far been so inadequate that vaccination remains virtually non-existent: “vaccination remains, for the moment, a privilege of the rich countries. A quarter of the 2.295 billion doses administered worldwide were administered in the G7 countries, which account for only 10 per cent of the world’s population. Only 0.3 per cent was administered in low-income countries,” according to WHO. “At the current rate of immunisation, it would take 57 years for low-income countries to reach the same level of protection as the G7 countries,” Oxfam said.
Clearly, this global health apartheid has strong reasons. The first is financial. Vaccines are expensive and the public finances of these countries, already undermined by neoliberal budgetary policies over the past four decades, have been further eroded by the financial support measures necessitated by the pandemic. There remains the possibility of forcing the pharmaceutical groups that produce vaccines to provide them at a much lower cost. There would be no shortage of arguments in favour of this solution: in addition to the state of need in which the world’s population finds itself, central states could argue that they largely financed the development of these vaccines, in order to suspend or override the patents that currently allow pharmaceutical groups to make huge profits. But the few voices that have been raised on this issue have provoked a unanimous indignant retort from Johnson, Macron, Merkel and others: contracts must and will be honoured! It is a way of reaffirming their attachment to the sacrosanct principle that, if costs are socialised, profits can only be privatised. This adds a new contradiction to the previous ones: if health is a public good and a right, it is today in the hands of private interests which, at least in part, can jeopardise it.